The concept of neurodivergence has become more visible in recent years and normalized, but many people still suppose it’s one diagnosis.
Neurodivergence doesn’t even exist as a diagnosis. It’s a term created to describe different neurological differences, so brain differences. These differences can be classified as a diagnosis (ADHD, OCD, autism, dyslexia, etc.) or a scattered set of signs that is insufficient to get a diagnosis.
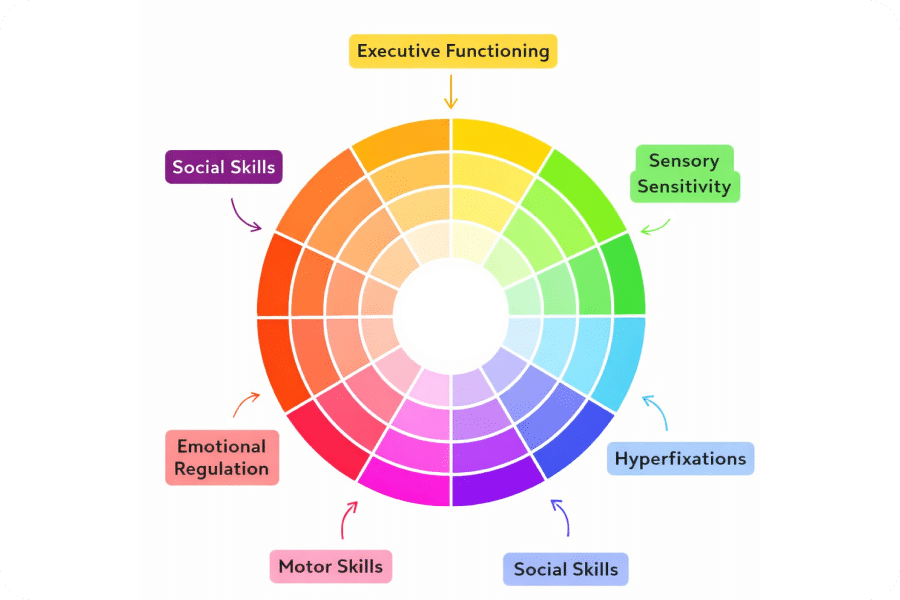
This is why neurodivergent people can be so different. In this article, we explore the most common parts of the neurodivergent spectrum. Feel free to use our neurodivergent spectrum chart to better visualize how neurological differences feel in practice.
What Is Neurodivergent Spectrum?
The neurodivergent spectrum is a wide range of natural variations in how human brains function.
Viewing neurodivergency as a spectrum is a much more inclusive concept. Since we started viewing neurodiversity as a spectrum, not a diagnosis, we stopped dividing people into “normal” and “other.” The “Am I neurodivergent?” quiz helps people to determine their place on this continuum. For example, some people may find out that they have neurodivergent symptoms in relation to motor skills and self-perception but have exceptional executive functioning.
Symptoms on the neurodivergence spectrum usually come in predictable pairs. These sets of symptoms are associated with neurodevelopmental conditions, such as:
- ADHD
- Autism spectrum disorder
- Dyslexia
- Dyspraxia
- OCD
- Tourette syndrome.
However, the spectrum concept focuses less on diagnostic labels and more on cognitive functioning. Two people with the same condition may show very different strengths and challenges because their traits appear in different domains.
Explaining the Main Components of Neurodivergent Spectrum
The neurodivergent spectrum is often easier to understand when we break it down into the following functional domains of the brain:
- Executive functioning
- Emotional regulation
- Motor skills
- Sensory sensitivity
- Social skills
- Hyperfixation (aka attention management)
These domains influence everyday experiences such as organizing tasks, regulating emotions, navigating sensory feelings, and paying attention.
An important note: while a neurodivergent person might experience intense feelings only in one domain, the challenges usually come in pairs. For instance, a person might have severe sensory sensitivity, which also makes them more susceptible to emotional dysregulation and executive dysfunction. This happens due to the connection between the brain’s sensory and limbic parts [1].
Executive Functioning
Executive functioning refers to a group of cognitive processes that help people plan, organize, and complete tasks. 89% of people with ADHD and 62% of those with autism experience at least one executive dysfunction symptom, research says [2].
Common executive functioning differences include:
- Difficulty starting tasks
- Losing track of time
- Being unable to organize
- Finding transitions hard
- Unable to focus
- Constant brain fog
Executive dysfunction can often be called “laziness.” However, executive dysfunction isn’t simply procrastinating. It’s a physical inability to do anything because the brain lacks certain chemicals.
Emotional Regulation
In the neurodivergent spectrum, emotions can sometimes feel more intense, rapid, or difficult to control than in neurotypical individuals. There are a lot of diagnoses that sum up these experiences: Rejection Sensitive Dysphoria (RSD), Oppositional Defiant Disorder (ODD), Sensory Processing Sensitivity (SPS), etc.
Emotional regulation differences on the neurodivergent spectrum mean that a person’s brain is more responsive to stimuli due to brain structure and functioning. Although it’s difficult, many neurodivergents learn to cope with their intense feelings due to therapy or self-care.
Motor Skills
In simple terms, motor skills are the coordination of physical movement, including maintaining posture and tying one’s shoes.
A little-known fact, but people on the neurodivergent spectrum can have difficulties with motor skills. These symptoms can show up as early as 12 months among young children with autism [3]. It can show up as:
- Clumsiness
- Slower reaction time
- Challenges with precise hand movements
- Toe-walking
- T-Rex’s hands while sleeping
Dyspraxia is a neurological condition where these symptoms are the most prominent. But similar traits can also appear in ADHD or autism.
Sensory Sensitivity
Neurotypical individuals usually filter out sensory noise, like a slightly higher temperature, the texture of their favorite drink, etc. But one part of the neurodivergent spectrum is experiencing smells, tastes, sounds, and textures more intensely because the brain is more sensitive to these irritants.
If you yourself are neurodivergent or know neurodivergent people, you might notice that some of them refuse food if some of the food tastes off. Or they might become angry when they are in a crowd, the sun is shining, they are wearing an uncomfortable outfit, and you require their attention. That’s sensory sensitivity showing up.
Social Skills
Neurodivergent individuals can struggle with social skills, hence, they are put on our neurodivergent spectrum chart. The reason why social situations can be a cause of a lot of stress for people on the spectrum is due to executive dysfunction. People with autism, ADHD, OCD, etc., don’t have enough resources to keep in mind conversations and decode multilayered social cues.
Hence, neurodivergent individuals may prefer more direct communication and literal language. Hints, sarcasm, implicit meaning, and non-verbal language can be hard for them to understand and repeat. It requires extra cognitive effort, tiring neurodivergents.
Hyperfixations
Hyperfixations are periods of intense focus on a specific interest. The stereotype that neurodivergents obsess over dinosaurs or trains actually has a reason. When a neurodivergent person has a topic, they can build their whole personality around this topic and indeed seem obsessive.
Hyperfixations are particularly common in ADHD and autism, where the brain’s dopamine system responds with dopamine bursts when a person engages in an activity that feels rewarding or stimulating. This can lead to remarkable expertise in specialized topics such as science, art, gaming, history, or technology.
At the same time, hyperfixations can make it harder to shift attention to tasks that feel less interesting or urgent. Time may pass quickly while focusing on the preferred topic to the point that neurodivergent individuals may even forget they didn’t eat or didn’t fulfill their work responsibilities today.

Why Knowing Your Place on the Neurodivergent Spectrum Is Important
For years, neurodivergent individuals have lived with labels such as “weird,” “clumsy,” “nerd,” etc. It may lead to self-destructive thoughts that something is indeed wrong with the person. It’s not an illustrative case, it’s a reality for many neurodivergents, especially undiagnosed ones.
Understanding where you fall on the neurodivergent spectrum can be a powerful step toward greater self-awareness. When you recognize yourself in neurodivergent traits, it validates your challenges. It says that there was nothing wrong with you, but your brain works differently in a world that wasn’t designed for it.
Self-knowledge also makes it easier to develop practical coping strategies. For example, someone who recognizes executive functioning challenges might use planning tools or take breaks more often. A person with sensory sensitivity may purchase specialized noise-canceling headphones and even file for workplace adjustments.
Ultimately, the goal of exploring your neurodivergence is not to place a limiting label on yourself. Knowing your place on the neurodivergent spectrum is about recognizing your strengths and weaknesses and treating yourself with compassion in areas where your brain needs help.
FAQs
Why Do Neurodivergent People Differ So Much?
Neurodivergence is called a spectrum because traits appear in different combinations and intensities across individuals. Two neurodivergent people with similar life experiences can experience totally different symptoms and, hence, be more or less functioning. Genetics, environment, upbringing, and personal experiences also impact how traits on the neurodivergent spectrum will show up.
Is ADHD on the Neurodivergent Spectrum?
Yes, ADHD is widely considered part of the neurodivergent spectrum. The main symptoms of ADHD, such as executive dysfunction, emotional dysregulation, and hyperfixations, are all part of the neurodivergent spectrum. It means that people with other neurodivergent conditions can also share ADHD-like symptoms.
What Is a High-Functioning Neurodivergent?
The term “high-functioning” is sometimes used to describe neurodivergent individuals who appear to be a stereotypical image of neurotypical. For example, a “high-functioning” neurodivergent can successfully manage daily responsibilities at work, school, and in relationships.
Positive things can make a neurodivergent high-functioning, such as a supportive environment, therapy, and accommodations. But some neurodivergents also use masking strategies and toxic motivations to meet social expectations.
How Do I Know If I Am Neurodivergent?
The most effective way to know if you’re neurodivergent or not is by referring to a mental health specialist. However, neurodivergent conditions are frequently underdiagnosed, so many individuals refer to online evaluations and psychological assessments.
You can also try to collect your family history or talk to other neurodivergents to try to understand yourself. Family, along with other neurodivergents, might share their knowledge and tips on how to find a definitive answer.
Sources:
- Linking irritability and functional brain networks: a transdiagnostic case for expanding consideration of development and environment in RDoC. Neuroscience & Biobehavioral Reviews. July 2021
- Executive function deficits in attention-deficit/hyperactivity disorder and autism spectrum disorder. Nature Reviews Psychology. August 2024.
- Motor Development in Children With Autism Spectrum Disorder. Frontiers in Pediatrics. September 2021.















