
A large percentage of college students suffer from anxiety or depression. JESHOOTS/pixabay)
Opinions do not necessarily represent CUIndependent.com or any of its sponsors.
Whether a student is struggling with suicidal thoughts, the aftermath of sexual assault or day-to-day stress and anxiety, mental health services should be easily accessible to everyone. These services are a necessity CU has taken too lightly.
As of 2013, roughly 40 percent of college students suffer from some form of anxiety, while 36 percent suffer from a form of depression, and a large majority of campus counseling programs have said the number of students with psychological problems is a growing concern.
A study conducted by UCLA sociology professor S. Michael Gaddis found that in places where peers stigmatize mental health treatment, students do not want to acknowledge, nonetheless seek treatment for, their mental health struggles. According to interviews with a select few CU undergraduate seniors, all agreed that the topic of mental health on campus has had a negative stigma during their four years at the university.
“One of my friends refused to go, even when he was struggling, because of the stigma,” said CU Boulder senior Mackenzie Brecker when asked why students might not seek out help on campus.
The university already struggles to juggle students who do seek out counseling and psychiatric services. Those who not only feel hesitant to utilize the resources provided on campus, also aren’t always given the comprehensive experience they deserve if they do.
According to an interview with Donald Misch, Senior Assistant Vice Chancellor for Health and Wellness and Executive Director of Wardenburg Health Services, Counseling and Psychiatric Services and Psychological Health and Psychiatry merged in 2015 in order to increase student access to mental health services and enable more students to take advantage of these resources on campus.
Over the last few years, CAPS has considerably improved mental health services at the University of Colorado at Boulder. However, while most students interviewed agreed that the services provided are helpful, most also agreed that they’re not comprehensive enough to meet the mental health demands of students.
“I had a great session, but I ended up seeking help elsewhere,” said one CU Boulder senior who spoke on the condition of anonymity. “While they were helpful, I felt like I was in and out really quickly because they just kind of placed me into a category and sent me on my way. It made me feel hesitant to go in and get help again.”
Students also expressed that their experiences hinted at a mental health hierarchy. If a student expresses suicidal tendencies, his or her case becomes a top priority for CAPS, and rightly so. However, because of the lack of resources, many students who are suffering from less severe day-to-day struggles are categorized into low-priority cases and are often passed on to intern counselors, or aren’t given priority in scheduling. Thus, students are not being given equal and fair access to proper and full services.
“It felt like they categorized my need for help as not severe […] and therefore, they assigned me to a training intern who basically told me she was unsure how to help,” said another CU student who preferred not to be identified. “They should categorize every problem as important.”
Currently, CU students pay a fee for six “free” visits to CAPS. In 2017, the student government leaders approved doubling what students pay to receive the limited free visits to the counseling center, to provide more services to students. Once the six “free” visits are up and a student wishes to continue using the services, a payment plan is established.
On the other hand, students who pay the $1,995 for the Student Gold Insurance Plan get up to 20 “free” visits with counseling services. However, this plan does not make up for the lack of resources, as students become increasingly frustrated by long waiting periods in between sessions, pushes toward group therapy, and the constant trade-off of counselors.
Some students have claimed that they might wait three to four weeks between sessions if the student isn’t a priority case. While walk-in times are available to students, the resources for consistent one-on-one work are still a problem, as students are pushed towards working out their issues in group therapy or with a new counselor every time they walk in.
According to students, most of those who have used the free visits and didn’t find them helpful stopped there, contributing to the growing concern that students feel discouraged when seeking out help. For those who do seek out help, paying $1,995 ultimately becomes obsolete when they use professional help off-campus and pay an additional $100-plus for comprehensive services, on top of their tuition costs and student insurance.
In addition, the city of Boulder does not have enough off-campus mental health professionals to meet the needs of students who are struggling with daily issues that need to be talked about.
In March 2014, Newsweek published a series of maps meant to show relative health by county across the nation. For every 2,000 citizens, there is one mental health provider in the Boulder/Denver area. Given that Boulder is a college town and, therefore, has a more populated and condensed population, this ratio becomes even more disparate.
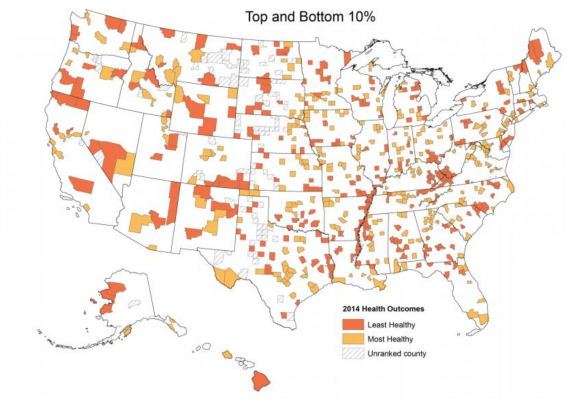
A map shows the highest and lowest levels of mental health in counties across the country. (Newsweek)
In 2013, the University of Western Georgia committed to improving students’ well-being by covering unlimited counseling services in student tuition — a change that has allowed for better accommodation to all students’ mental health needs.
Currently, the CU student tuition breakdown for both out-of-state students and in-state students consists of undergraduate mandatory fees that include an athletic fee, a capital construction fee, a recreation center expansion fee, and a student activity fee, all of which concern CU athletics. These fees make up 66 percent of the mandatory fees.
On the other hand, only one fee exists specific to mental health, making up 4 percent of the mandatory fees.
Additionally, the University of Western Georgia has created a program in which the counseling center joins with peer mentors, creating an indirect peer-to-peer outreach arm. This student advocacy and outreach work for mental health improvement among the student body creates an open and safe environment for dialogue about mental health — another feature CU has failed to address with mental health.
Of those interviewed, most students agreed that the university does not provide an open and safe environment regarding mental health issues. Most students who have not utilized CAPS haven’t done so because they think they aren’t in need of the services due to the stigmatized notion that counseling is only for severe mental issues.
However, counseling, simply put, is guidance. Most students interviewed also agreed that one of the biggest improvements on campus, in regards to the mental health services, is awareness. Due to the current lack of outreach and advocacy, and the prioritization of physical health and athleticism over mental well-being, CU Boulder neglects the thousands of students in need of a more comprehensive CAPS program.
“I don’t need three racquetball rooms [… ] I need guidance,” said one student when asked if tuition fees should go to mental health services over other features of the university.
If the university were to redirect the $600 that currently goes toward athletic upkeep to mental health services, CAPS could make major improvements toward providing all students with the services they deserve.
Contact CU Independent Staff Writer Alex Segell at alexandra.segell@colorado.edu
